Cancer Basics
Here are some general principles (which have many exceptions) that can be used to describe "cancer" as a whole. Let's talk about some cancer basics.
There are few diseases more feared by patients around the world than cancer. In the United States, cancer is the second most common cause of death after heart disease. It can attack any part of the human body, from your lungs and brain to breast and bone. Not only is the disease itself universally dreaded, but so are many of the treatments. When you picture a bald young woman suffering from breast cancer, much of the agony you perceive is a side effect of the medications saving her life.
Despite the fear around cancer, it's not a disease that is well understood by the public. Society uses the word "cancer" to describe thousands of different tumor types, all with very different pathologies, treatments, prognosis, mutations, and outcomes. It's NOT one disease.
Take lung cancer for instance. Not only is it extremely different from breast, pancreatic, and prostate cancer, but it's also an umbrella term for many different tumor types. Lung cancer itself can be broken into non-small cell lung cancer (NSCLC), small cell lung cancer, carcinomas, sarcomas, and others. You can even have cancer in your lungs that came from somewhere else (known as metastasis), which wouldn't be considered "lung cancer" at all. Within NSCLC alone exists adenocarcinoma, squamous cell carcinoma, and large cell carcinoma, ALL OF WHICH ARE TREATED DIFFERENTLY. The "cure for cancer" is a fairytale that will never exist, because these diseases are far too different.
Having said that, there are some general principles (which have many exceptions) that can be used to describe "cancer" as a whole. Let's talk about some cancer basics.
You'll often see the following cancer basics described as "The Hallmarks of Cancer" in the literature. The hallmarks we'll cover today are mutation, growth, inflammation, invasion, immune evasion, and metabolism.
Mutation
Genomic instability allows for the accumulation of mutations in cellular DNA that ultimately allows cancer cells to thrive. In normal cells, mutations are repaired through a number of mechanisms and cell cycle checkpoints. This insures that defective cells cannot replicate and that oncogenic cells undergo apoptosis (cell death). One of the most important genes in this process is p53, which is often mutated in tumor cells. There are many different mutations that can occur, some of which are shown in the image below.

In cancer, DNA repair mechanisms are hindered which allows damaged cells to replicate and mutate. This instability causes a high mutational burden in cancer cells and ultimately acts as fuel on an evolutionary fire. For instance, mutations that enhance growth and cell survival will be replicated. Additionally, many tumors are made up of a genetically diverse population of cells which makes them harder to treat.
Growth
All cells need to be able to grow. They do this by responding to growth factors which attach to a variety of growth factor receptors on the cell surface. One classic example of this is the epithelial growth factor receptor (EGFR).
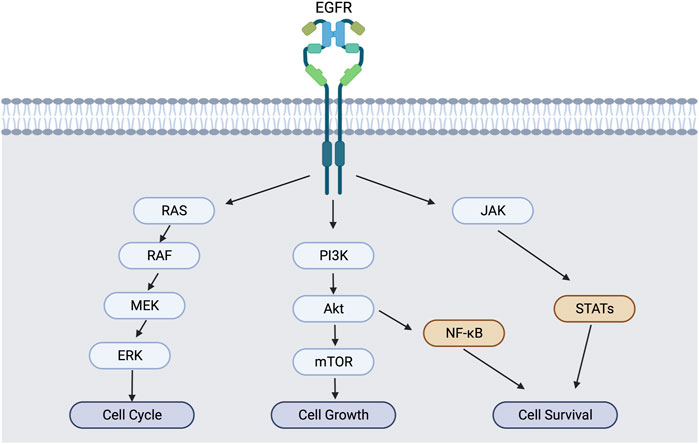
Cancer cells secrete growth factors, over produce growth factor receptors, and often have mutations in their growth factor receptors that cause uncontrolled growth. They do all of this while harboring levels of DNA damage that would kill most cells due to its ability to alter DNA repair mechanisms as described previously.
Inflammation
Inflammatory responses are a necessary part human biology and the immune system in particular. The innate immune system can cause transient inflammation in response to an injury, which ultimately allows for tissue repair. Once the injury has been repaired, inflammation decreases.
On the other hand, inflammation can also cause DNA damage, which can add to the genomic instability associated with cancer. This is likely why chronic inflammation and related comorbidities like diabetes have been correlated with increased cancer risk. Inflammatory immune cells can supply growth factors to cancer cells causing tumor growth, and they can also trigger angiogenesis and metastasis.
Invasion
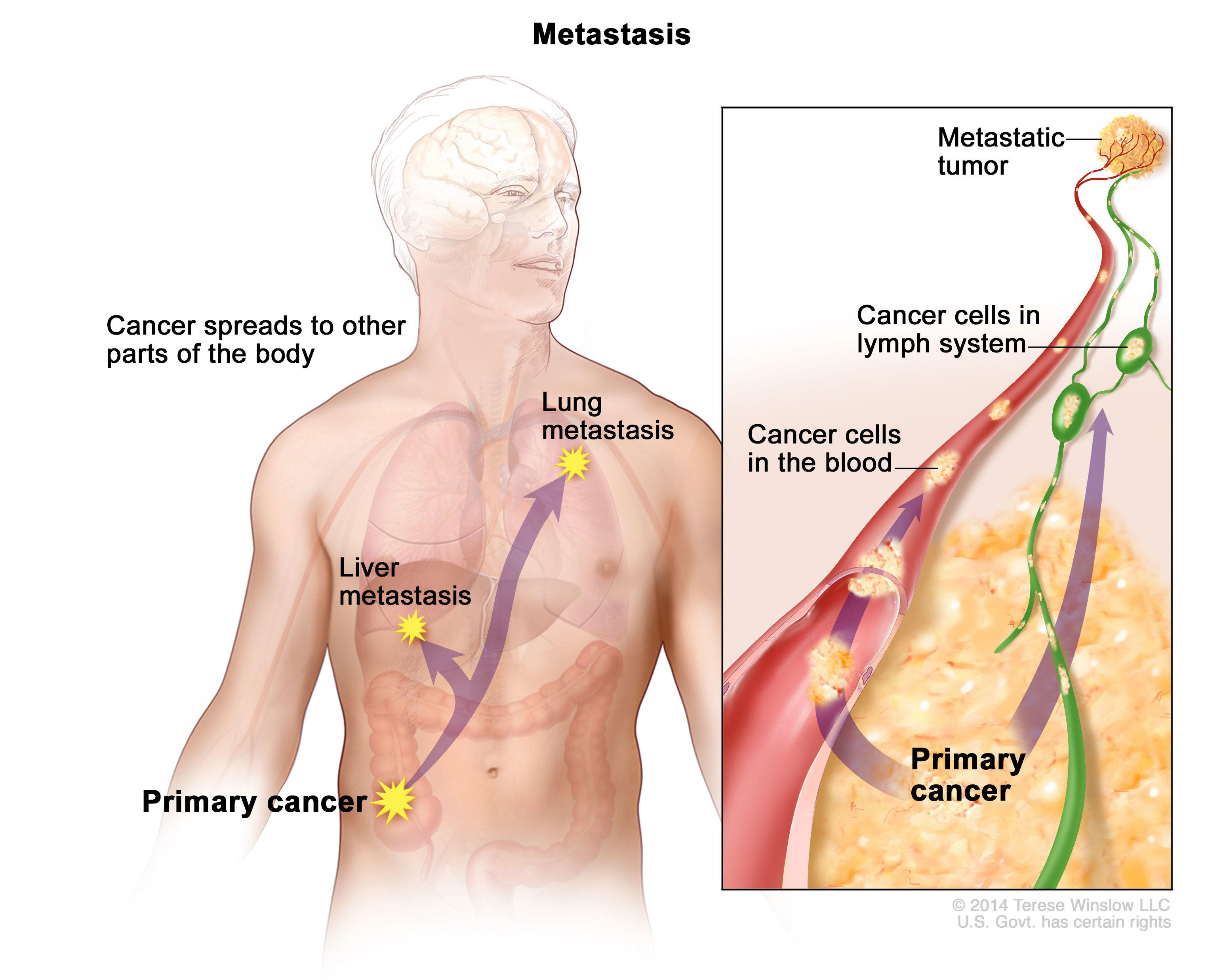
As I mentioned in the introduction, cancers have the ability to spread to other tissues in the body which is known as metastasis. The areas in which cancers metastasize depends on the cancer type and primary location. For instance, EGFR mutated lung cancer tends to metastasize in the brain more often than other types of lung cancer. When a cancer spreads to other areas of the body, it is generally considered "advanced" and also comes with a poor prognosis compared to tumors caught before they spread.
Immune Evasion
One of the largest leaps forward in cancer treatment has been the development of ways to utilize a patient's own immune system against their cancer. Unfortunately, cancer cells are very good at hiding and they do so through a number of mechanisms.
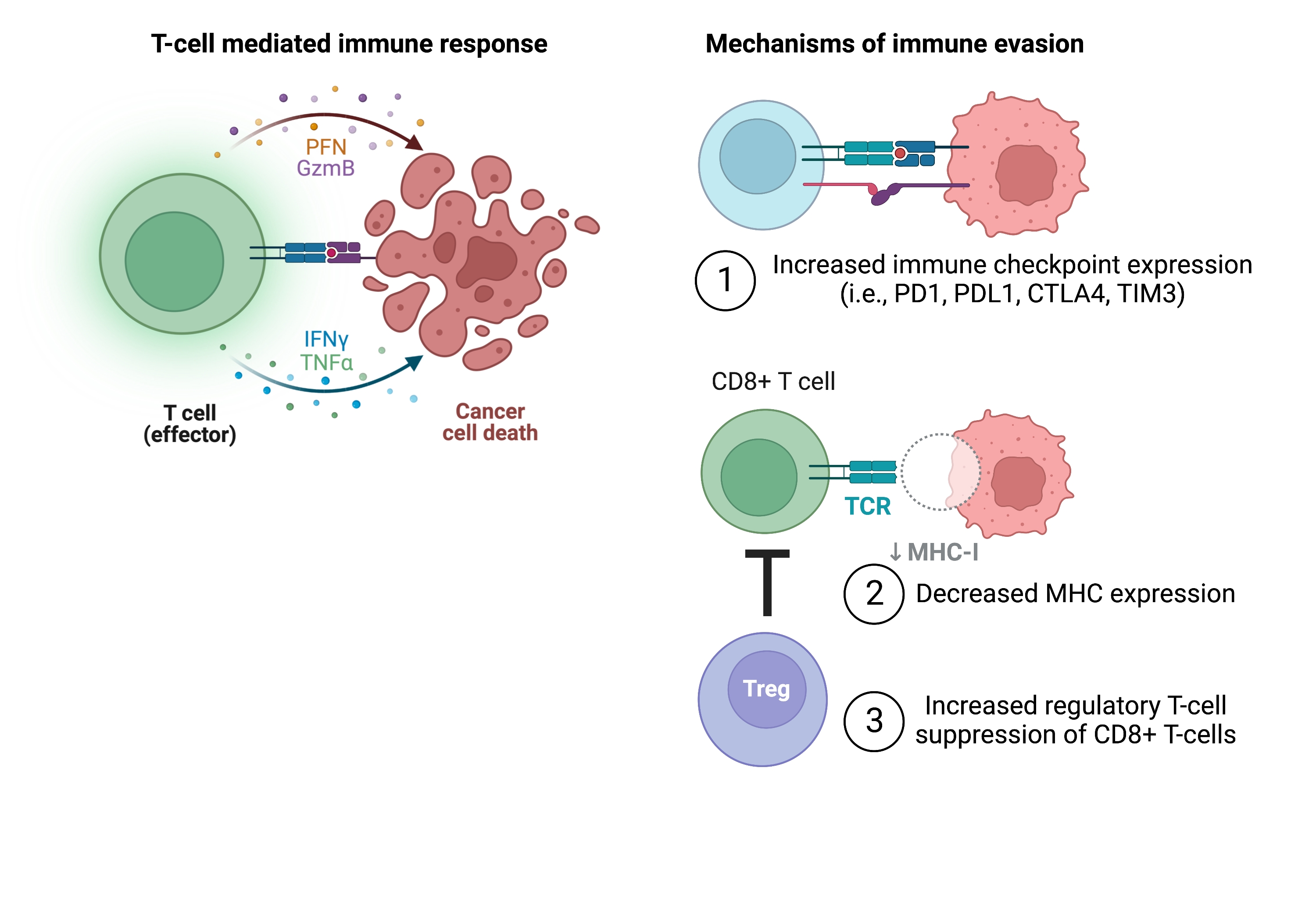
Cancer cells must avoid detection by the immune system in order to survive. They do this by increasing or decreasing the expression of certain peptides and by recruiting other immune cells that are normally their to regulate the immune response. In other words, cancers take advantage of mechanisms that already exist in your body that would normally prevent out of control immune responses and autoimmune diseases.
Metabolism
Last but not least, we have metabolism. We've talked a lot about metabolism on RxTeach when it comes to Zone 2 training, diabetes, and mitochondrial health, but it also plays a huge role in cancer.

The important thing to remember here is the "Warburg effect" which essentially states that cancer cells use anaerobic glycolysis to create energy rather than oxidative phosphorylation as shown in the image above. In other words, much less pyruvate will undergo mitochondrial respiration in cancer cells compared to healthy cells.
This is actually a much less efficient way to create energy, so cancer cells must utilize a disproportionate amount of glucose compared to normal cells. This is why we use PET scans to find cancer. A radioactive glucose analogue will show up on a PET scan at higher concentrations in cancer cells than normal cells due to the Warburg effect. Pretty cool.
I hope you've learned a little bit about cancer and how it works! This is a very complex disease, but I think an enhanced understanding by the general public can only be a good thing. Make sure to subscribe to RxTeach so you don't miss upcoming articles on cancer!
*Information presented on RxTeach does not represent the opinion of any specific company, organization, or team other than the authors themselves. No patient-provider relationship is created.

