A Sliver of the Liver: Key Concepts in Hepatic Function
The liver, often overlooked alongside the kidneys, is a vital organ for metabolizing medications and toxins, producing bile to emulsify fats, and storing energy as glycogen, among many other functions.
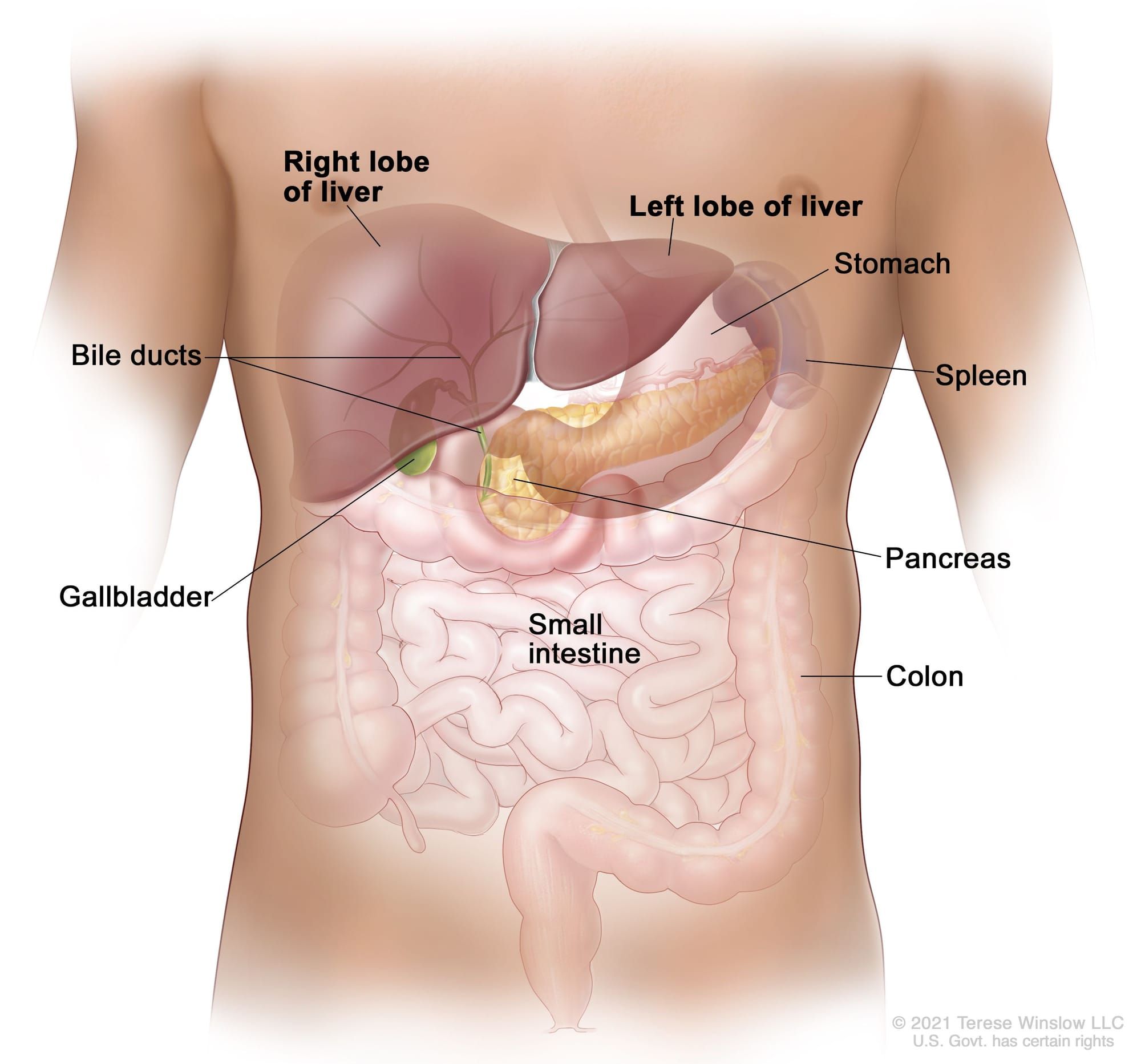
The liver, often overlooked alongside the kidneys, is a vital organ for metabolizing medications and toxins, producing bile to emulsify fats, and storing energy as glycogen, among many other functions. It's also the largest internal organ in the body, so take that, kidneys, bigger is always better.
Despite its size and critical role in normal physiology, the liver often takes a back seat. This is largely due to the heavy spotlight placed on the kidneys, driven by the routine need for renal dosing adjustments in everyday practice. Hepatic considerations, on the other hand, are encountered less frequently and require more nuanced interpretation.
Hepatic Impairment
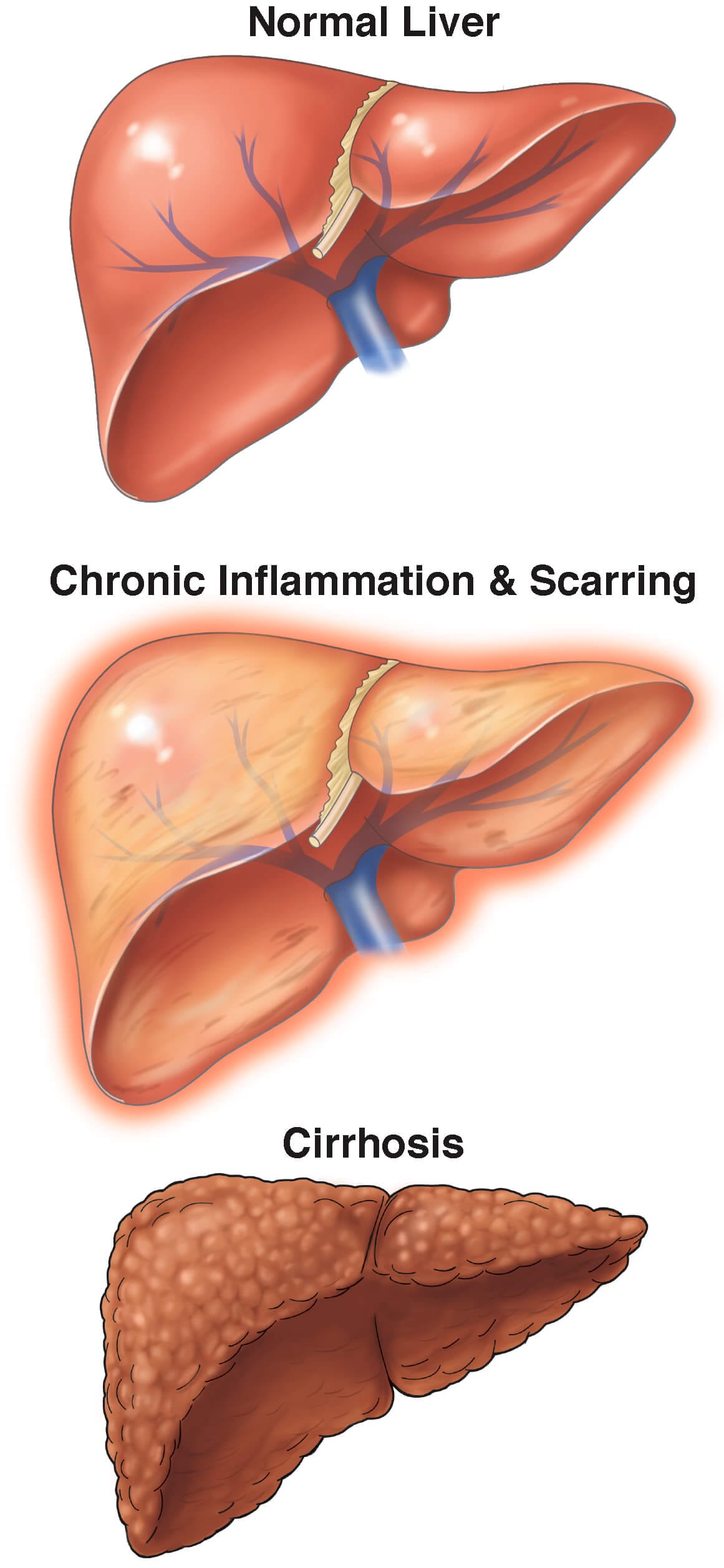
Unlike the more straightforward assessment of renal function using creatinine clearance or glomerular filtration rate, hepatic function is less intuitive. Tools such as the Child-Pugh score attempt to stratify liver disease severity and guide dosing recommendations by incorporating the following:
- Laboratory values such as total bilirubin, albumin, and INR
- Clinical presentation of ascites and encephalopathy
Drug interactions:
The Cytochrome P450 (CYP450), found in hepatic and intestinal cells, is a widely encompassing group of enzymes responsible for the metabolism of a vast number of biochemical compounds, including medications. Some of these enzymes include CYP3A4, CYP2D6, CYP2C9, and CYP1A2. These enzymes introduce patient-specific variability, not only when you consider differences in natural enzyme function through genetic differences and expression levels, but also because many enzymes can become inhibited or induced by medications, foods, and even cigarette smoking.
Enzyme inhibition or induction can drastically alter drug exposure, and for non-prodrugs generally follows:
- Inhibitors → increased drug levels → potential toxicity
- Inducers → decreased drug levels → reduced efficacy
For example, fluconazole, an antifungal agent, is a strong inhibitor of many CYP enzymes and can elevate concentrations of warfarin, an anticoagulant, placing patients at a higher risk of bleeding.
For pharmacists, this is where pattern recognition becomes essential. Identifying high-risk combinations and anticipating their impact is a critical skill in maintaining patient safety.
First-Pass Metabolism
Oral medications, like food, are absorbed through the gastrointestinal tract and transported via the portal circulation directly to the liver for initial processing. For medications, a significant portion may be metabolized before ever reaching systemic circulation, ultimately decreasing our "F" or bioavailability fraction. For this reason, we must consider dosing adjustments when switching between our oral and parenteral administration routes! It should be noted that not all medications are significantly affected by first-pass metabolism.
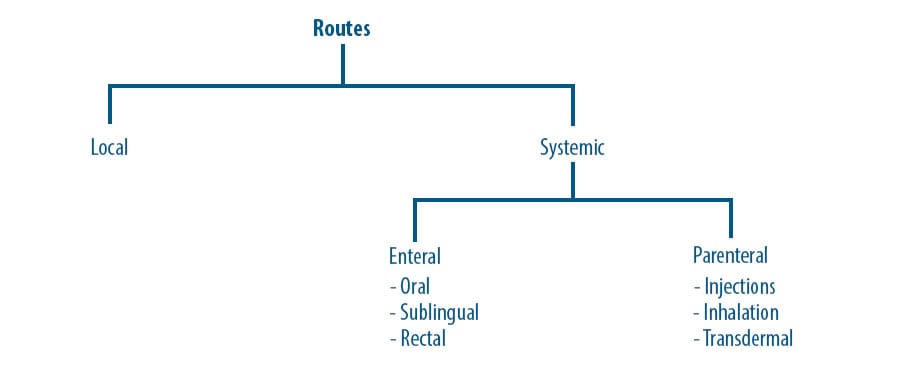
One easy example is opioid medications, where we commonly convert between morphine milliequivalents to standardize doses by relative potency of agents. According to Lexi-Drug, oral morphine has a bioavailability of 17 to 33%. For this reason, we commonly equate 30 mg of oral morphine to 10 mg of IV morphine, both of which lead to comparable systemic circulation levels and hopefully pain control.
Other physiologic roles
The liver has a role in producing key proteins and regulators in normal physiology, with some tying back to the aforementioned Child-Pugh score.
- Albumin production → affects drug protein binding
- Clotting factor synthesis → relevant for anticoagulation management
- Bile production → essential for fat-soluble vitamin absorption
Albumin significantly impacts pharmacokinetics, with many drugs binding to it for transport through the bloodstream. Decreasing albumin levels can increase the free fraction of highly protein-bound medications, potentially enhancing both efficacy and toxicity. An easy example is phenytoin, an antiepileptic with a narrow therapeutic index, which is approximately 90% protein-bound and has its own calculation to estimate free drug concentrations!
Additionally, the liver acts as a detoxification hub, converting lipophilic substances into more water-soluble compounds for renal elimination or also transporting waste into the intestines for fecal elimination. When this system is compromised, accumulation and adverse effects become much more likely.
I hope this article gives you a newfound love and appreciation for the liver! There are so many ways altered hepatic function can impact clinical decision making, and it deserves the occasional spotlight attention as far as I'm concerned. Have a great rest of your week!
References:
*Information presented on RxTeach does not represent the opinion of any specific company, organization, or team other than the authors themselves. No patient-provider relationship is created.

